This eBook explores the benefits of:
-
Shifting payment integrity from recovery to prevention
-
Connecting prepay and postpay efforts for stronger payment integrity
-
Leveraging payment integrity AI efforts mindfully
Nearly 20% of the U.S. gross domestic product (GDP) is expected to be spent on healthcare costs by 2032. For perspective, that’s akin to the economy of entire countries, like Japan or India. And with a significant portion of the Baby Boomer generation yet to age into Medicare, those costs alone are expected to balloon to over $7 trillion by 2031.
Part of the reason for these high costs is that healthcare is complex. Fragmentation, mounting costs, and constantly evolving regulations are a challenge across health plans, patients, partners, and providers. With these complexities and the volume of healthcare claims on the rise, improper claim payments show no sign of slowing down. Indeed, for 2025, the Comprehensive Error Rate Testing (CERT) program showed an improper payment rate of 6.55%. That’s potentially $400 billion of waste each year just within Medicare and Medicaid.
Another result of these economics is that health plans’ medical loss ratios (MLR) and administrative loss ratios (ALR) are simultaneously on the rise. The Affordable Care Act requires an MLR of about 80–85%, but due to the rising costs of care, regulatory changes, and other factors, the largest health insurers are seeing MLRs rising to an average 88% while many smaller and midsize plans’ MLRs climb even higher. ALRs are hovering between 11% and 13%. As a result, very little room is left for profit margin, and total cost management is at the top of every payer’s corporate goals.
What is the solution?
Payment integrity is potentially one of the biggest total cost management levers for health plans. They must create payment integrity programs that can scale, grow, cut through complexities, and increasingly rely on technology to automate where possible while making necessary expert human review as efficient as possible.
Future‑proofing payment integrity demands a fully connected ecosystem with the right technology and logic that allows organizations to leverage automation and prevention intelligently, integrate prepay with postpay for comprehensive oversight, and engage as early in the payment continuum as possible. This fully connected ecosystem relies heavily upon proper data orchestration and the responsible use of AI to shift from simply reacting to problems to preventing them—while maximizing both medical and administrative savings along the way.
In this eBook, we will walk through the current challenge areas for errors, waste, and abuse, common pitfalls of payment integrity efforts, and key solutions in moving toward a more holistic system that connects prepay and postpay integrity all along the claim payment continuum.
Challenges with the current state of payment integrity
Today’s healthcare payment system features many moving parts. There are several payment models: fee-for-service, bundled service, case rate, per diem, value-based payments, and others. There are numerous settings where care takes place: from primary care and dental offices to emergency department and inpatient to outpatient to skilled nursing facilities. And there are numerous entities performing the care itself: doctors and dentists performing procedures, labs running tests, durable medical equipment companies outfitting patients, and pharmacies dispensing drugs. On top of that, the facilities and entities each send separate claims to the payer.
The revenue cycle process involves multiple and siloed systems: from eligibility and prior authorization, to billing and claim routing, to claim adjudication and electronic payments. This overlapping and complex system is ripe for errors, waste, abuse and even fraud, including instances such as:
-
Duplicate claims, over-coded claims, and incorrectly coded claims
-
Diagnostic related group (DRG) claims that don’t match the medical records
-
Inpatient readmissions that are improperly billed
-
Anesthesia claims for a prior claim denied as elective
-
Claims for services never rendered
-
Suspicious patterns of abuse by specific providers
The list of potential for improper claims is endless. When and how a payment integrity system can and should intervene along this revenue cycle varies greatly by claim scenario. While payment methodologies, complexity of claim sequencing and repricing, provider contract terms or other levels of prepay exclusion may require some level of postpay review, we at Cotiviti estimate that payers could shift up to 70% of their payment integrity before claim payment while still catching significant overpayments in postpay audit and recovery (see Figure 1). But that shift is not always simple. Let’s go through just a few of the challenges of shifting more to prepay while keeping a strong postpay safety net:
Fragmented data: Gaps in claim review process integration and incomplete data sent to multiple payment integrity solutions are all cumbersome challenges to scaling up payment integrity efforts beyond postpay audit and recovery or core claim editing. For example, missing just a few key inpatient data fields in a prepayment integrity file layout could dramatically limit the ability to spot improper claims.
Incomplete analytics and technologies: Many plans may overlook critical opportunities for cost containment because these functions require consistent upkeep, clinical oversight, or strong technological connectivity. Is coordination of benefits (COB) validated before editing takes place? Is there a second‑pass editor to check more clinically complex scenarios? Are enhanced DRG and clinical reviews looking at higher-volume claims? All require a certain level of prowess and technology.
Lack of resources for policy maintenance: Another major prepay challenge is the clinical and technical time and resources needed to keep clinical policies and associated rule content current. More than 90% of client policies require updates every year—including those grounded in National Correct Coding and other industry standards—and when policies lag, claims slip through that should have been paused, flagged, or repriced, leaving substantial recoverable dollars on the table. Similarly, COB programs are rendered inefficient when plans rely on incomplete, inaccurate and/or outdated information.
Lack of human experts: While automated claim intervention takes care of a large portion of errors and waste, human interventions are still required to catch more nuanced improprieties and abuse that automation cannot, including some COB issues, modifier misuse, or outlier providers. Many inpatient and some professional and outpatient claim scenarios can’t be decided without also using medical records to validate an improper claim or pattern of claim FWA. Most plans simply can’t staff the number of humans with the skillsets and clinical claim knowledge essential for high-volume claim review.
Disconnected prepay and postpay: While many have begun to shift left and invest in prepay efforts, the disconnect of these efforts with traditional postpay models creates another challenge. Instead of gleaning findings and correcting gaps across the continuum, these efforts remain siloed, compounding confusion and adding to complexities that could be simplified.

Figure 1. Benefits of shifting from postpay to prepay.
Eliminating the above friction points requires a reimagined approach: one that embraces integrated prepay and postpay workflows, advanced analytics, and strategic clinical partnership to prevent leakage before it occurs.
Getting smarter about connecting postpay and prepay
Health plans need solutions that maximize value now, from prepay to connected postpay, while setting up programs for future growth. But even if an organization overcomes the technical and clinical challenges outlined above, shifting from postpay recovery to prepay prevention can still bring problems—either applying too much prepay pressure too quickly, creating abrasion with high‑value providers, or moving too slowly and delaying savings.
A smarter approach requires balancing different intervention types of prepay automation, prepay pause-and-review, prepay chart review, prepay pattern monitoring, and postpay review. Let’s examine how a few different improper readmission claim examples would require different prepay intervention types.
Automatic claim line denial: Automated reviews can detect improprieties in near real-time for efficient and accurate claim decisioning. Say that a patient was admitted as an inpatient to the hospital from the emergency room with a diagnosis of chronic obstructive pulmonary disease (COPD) exacerbation, treated, and discharged home. Ten days later the same patient was admitted to the same hospital with the same diagnosis of COPD exacerbation and received the same DRG assignment. Per CMS guidelines, the second admission was preventable and should be denied automatically as being related to the first admission, provided the editing system has all the right data elements coming in.
Claim line denial by pause-and-review: Although claim editing can apply readmission policy edits automatically, pausing and having claim history confirm that there was no other reason for the second admission gives some plans extra assurance. For example: a patient was admitted as an inpatient to the hospital following a car accident with a diagnosis of a concussion, was treated and discharged, and three days later the same patient was admitted to the same hospital, this time with an X-ray proven diagnosis of a pneumothorax (punctured lung). After claim history review, it was determined that the lung puncture was present (but missed) on the first admission, and the second admission is appropriately denied as being related to the first admission.
Prepay claim denial with chart review: Some prepay claims need to be supplemented with chart review for further context. As an example, an auditor noted that the discharge plan and instructions, which included starting a critical medication for pulmonary embolism, were insufficient. A prescription for Eliquis should have started the day of discharge of the first admission, however it was written to start a week later resulting in a gap in treatment. Due to the patient not receiving adequate treatment post-discharge and representing with the same symptoms during the subsequent admission, readmission is appropriately denied.
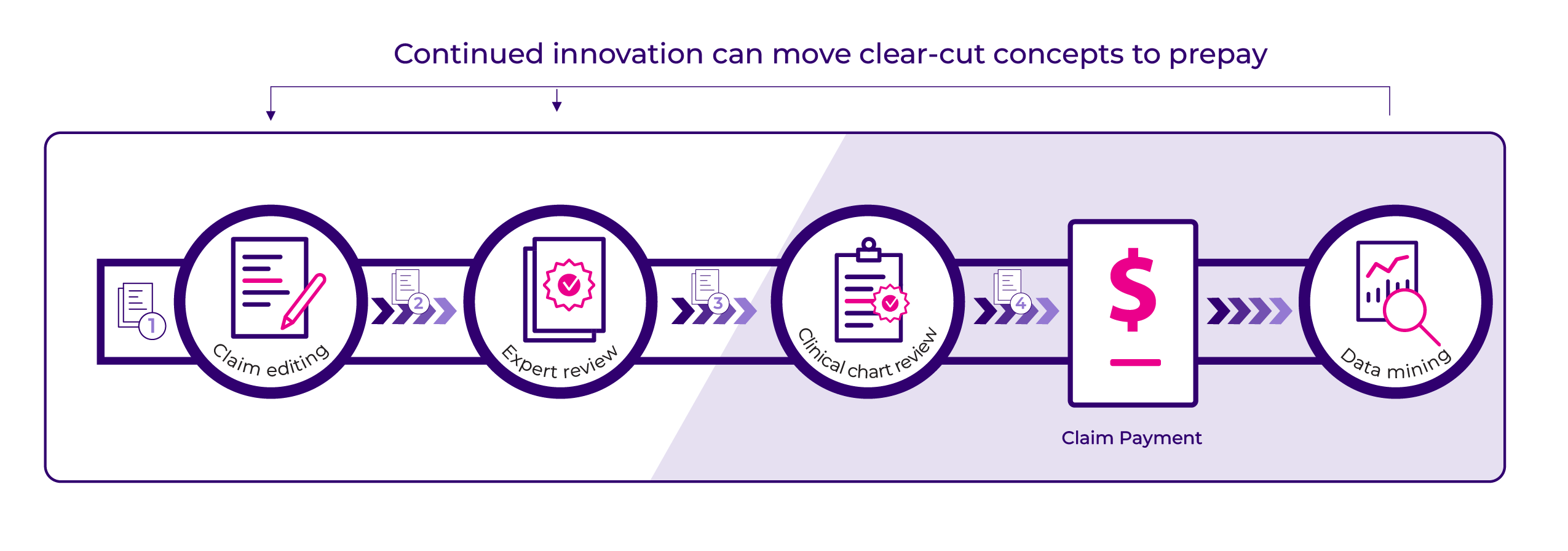
Figure 2. Example of different intervention types used for different readmission claim scenarios.
Many more review areas that have traditionally been postpay can be considered for shifting left. In early 2025, Cotiviti performed a comprehensive review of postpay Data Mining concepts involved in $2.5 billion of positive annual audit findings, linking those findings to prepay to-be-adjudicated data to assess the feasibility of shifting content across the payment continuum. Attributes such as repricing, contract compliance review, health plan reimbursement policy interpretation, complex client adjudication system reviews, and other operational considerations were evaluated to identify where differentiated actions could occur.
The findings were substantial. Based on Cotiviti data, 5–10% of value could move to a fully automated prepay intervention where data is available and reliable. Furthermore, 25–40% of value could shift to a prepay pause-and-review strategy where data is reliable but human review is still required for validation, using contract interpretation or situational context but without the need for medical record review.
In the end, a combined prepay and postpay approach has the potential to increase total improper dollars saved by up to 37% due to better conversion rates and increased catch rates within prepay review. In addition to higher recovery rates, plans can benefit from reduced provider abrasion and administrative cost by avoiding recoveries or offsets and the burdensome processes involved (e.g. provider letters, claim rebilling and reprocessing, back-and-forth phone calls, etc.). The time to value can also be accelerated as overpayments are identified pre-payment, instead of a possible 120 days or more post-payment.
Building effective payment integrity technology systems
Connecting prepay efforts with postpay efforts requires alignment, with clean data and shared systems using the same information seamlessly. Connected platforms using realtime data exchange, and scalable automation enable earlier detection, more accurate edits, and seamless transitions between prepay and postpay workflows.
To enable this ecosystem, technical and data gaps must be addressed to ensure meaningful analytics and interventions based on complete, accurate information. For example:
-
Crucial data elements in file formats that feed prepay payment integrity solutions are often missing and must be addressed, including outpatient, inpatient, drug or other claim types; member matching data; or accurate member eligibility, to name a few
-
Workflows for split-billed sequencing issues like those highlighted in global surgery guidelines need to be reworked for prepay
-
Separate repricing needs to be integrated for the automated ability to apply allowed amounts where the claim error is with pricing
-
-
Claim pend capabilities need to be added to prepay workflows for effective pending and retrieving of documentation when applicable, and that doesn’t exceed prompt pay guidelines
- New recommendations from payment integrity solutions must flow back into payer systems seamlessly, without heavy configuration, complex integration, or administrative strain on the health plan
-
Provider contract terms need to be accessible to payment integrity systems and expert reviewers
- Interoperability between electronic medical record (EMR) and payment integrity systems will become even more critical to ease administrative burden
-
Postpay intervention concepts must be comprehensive, and the synchronization with different prepay intervention systems must be tight, because without both, there will either be a lack of expert intervention ideas to shift left, or limited ability to shift them
A strong connected prepay and postpay system also incorporates effective and responsible use of AI. AI enhances capabilities by helping to better identify patterns, summarize complex medical documentation, and support claim and policy decision-making. That said, AI is a tool, not a solution. In healthcare especially, AI should not replace human expertise. Plans should look to strategically limit AI automation to enable human specialists to improve performance and outcomes. This means not replacing human clinical decision-making or judgment. Organizations can use AI to help prepare clinical content, but not to make decisions based on that content.
When a connected prepay and postpay system is applied with the right technology, data orchestration, mix of interventions, and responsible AI use, Cotiviti believes an organization can expect some 70% or more of their payment integrity program running in prepay mode, where the remaining 30% postpay is dedicated to tackling the most difficult scenarios such as retroactive data changes, sequencing and repricing, specific provider exclusions, or prior-authorization limitations.
Lowering both MLR and ALR
A connected payment integrity system also serves to help lower both medical costs and administrative costs. While postpay solutions are needed to catch a portion of inappropriate payments, payers are typically only able to recover 60–70% of the funds that were incorrectly disbursed. This is because the administrative work required to communicate findings and recover overpayments is expensive and inefficient for both payers and providers. Recovery costs for both payers and providers are estimated at upwards of $25 per overpaid claim, limiting the ability of payers to capture smaller overpayments and reducing the value capture by an additional 10–20%.
By catching issues earlier, catch rates and conversions are higher, which directly reduces medical spend and helps stabilize rising MLR. At the same time, administrative work becomes far more efficient, with fewer retroactive adjustments and less back-and-forth with providers. This combined effect creates a more predictable, sustainable cost structure across the organization.
The path forward for payment integrity
With a truly connected prepay and postpay system in place, what’s next for payment integrity? Earlier interventions in the claim payment process will be key to the future of payment integrity. These pre-adjudication or pre-emptive measures will complete the picture and substantially reduce administrative costs for both payers and providers by ultimately producing cleaner claims (see Figure 3).
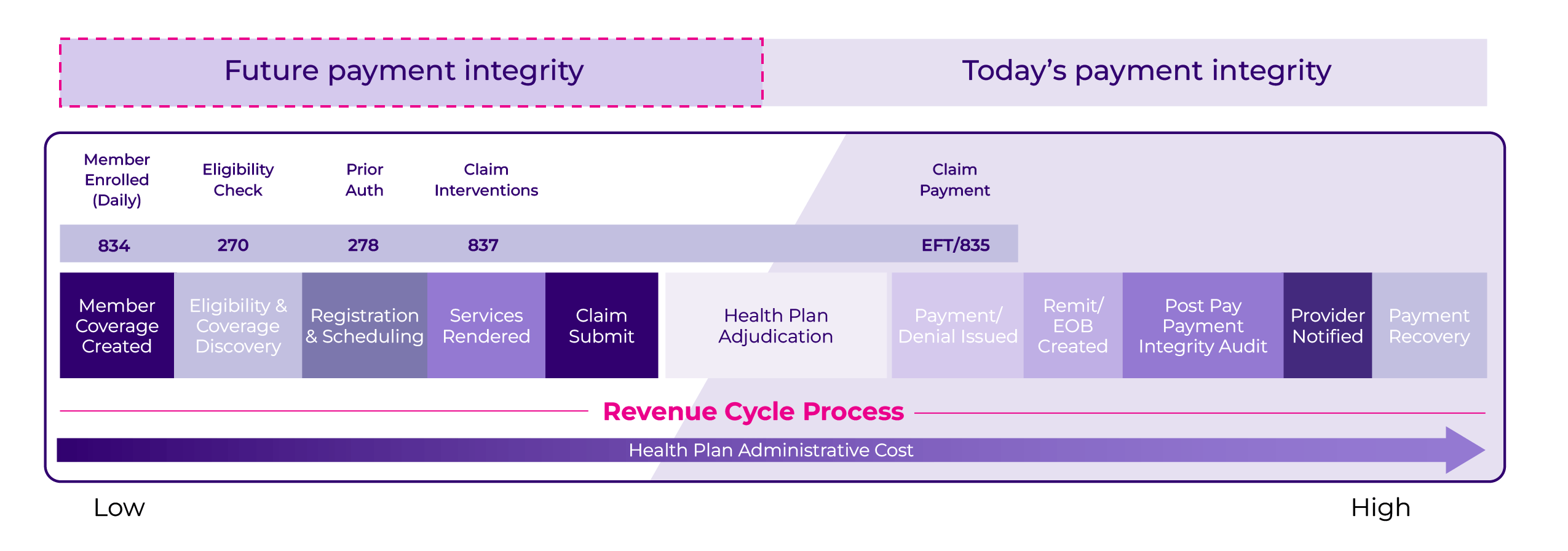
Figure 3. The possibilities for future payment integrity interventions shifting left.
Payers should be looking to move from purely vertical and isolated touchpoints to a continuum of intervention points that seek to do the following:
-
Intervene at the earliest point for the most impact
-
Accelerate value realization through multiple interventions delivered through a common platform
-
Integrate into existing workflows and complement existing solutions
-
Infuse AI into interventions and build self-correcting and learning processes
-
Leverage data and avoid creating new data silos
-
Deploy with the least amount of uplift to existing infrastructure
-
Address high-probability adjustments early, lowering provider friction.
-
Leverage and orchestrate data to provide unique insights across a variety of core client issues, including payment, administrative, risk, and quality
-
Seamlessly support decision making and intervention across preventative, prepay and postpay solutions with consistent results and provider experience
Coupling advanced analytics like machine learning and AI with robust data orchestration creates possibilities for scalable payment audits and reduced MLR and ALR. It is critical to blend this technical innovation with expertise and experience to close gaps, strengthen provider relationships, and maintain a high level of confidence in the accuracy and defensibility of early interventions.
Ultimately, future-ready payment integrity is about creating a cleaner, interconnected, and more transparent claim payment continuum. Plans that invest in this complete, connected approach will be positioned to adapt, evolve, and lead as the healthcare landscape continues to change.